SINGAPORE, Nov 22 — It is not every day that you can say you have five plump maggots wriggling on your palm by choice.
The sensation was not entirely unpleasant but the thought that these creatures could feed on human flesh was revolting.
In layman speak, these maggots were finding this writer’s palm unappetising and were leaving it alone, because they much prefer decaying flesh.
The creepy crawlies were courtesy of Carl Baptista, the laboratory director of Cuprina Private Limited, a home-grown medical device company that manufactures and supplies medical-grade maggots.
TODAY was touring the lab to find out more about the elaborate manufacturing process needed to breed the maggots, which are used to eat up the rotting flesh of patients whose wounds cannot heal, thus potentially saving them from having their limbs amputated, for instance.
For patients who undergo such treatment, the number of maggots placed into their wound are in the hundreds, and the quantity varies according to how bad the wound is.
Baptista, 45, whose background is in biotechnology and who has conducted research in the field of entomology, said the maggots that hatch from the lab’s sterilised eggs do not behave any differently from regular maggots.
“They have only one purpose. When they hatch, they look for food. As long as you give them food, they behave in the same way, whether the food is a sliver of meat or a chronic infected wound,” he said.
Maggots are able to distinguish between healthy and unhealthy tissue on a biochemical level, and actively seek out and consume necrotic (dead) tissue from wounds.
The concept of using maggots to clean and treat wounds is not new, and is one of the oldest forms of medicine.
The idea is for the maggots to feed on dead tissue, leaving behind healthy tissue to facilitate better wound healing.
Maggot debridement therapy is used to treat and heal certain chronic wounds that have extensive areas of dead tissue.
In Singapore, Baptista said that the treatment is not widely accepted at the moment, mainly due to the “yuck factor”.
“Much of the yuck factor comes from people’s imaginations. Not just patients may find it yucky but clinicians, when they first start out, find it yucky, too.
“But over time, when they see how useful maggots are as a tool (for chronic wound management), their confidence then gets imparted to the patients,” he said.
What is in the lab
On a weekday afternoon when TODAY visited the lab, 20,000 flies were hard at work.
They are the native bronze bottlefly species, the Lucilia cuprina, and they were housed behind double-walled glass doors in a negative-pressure lab where the temperature and humidity were controlled.
Some were feeding on liquid food consisting of vitamins and sucrose; others were slurping up a protein substrate.
The sexually active ones were buzzing around decomposing sheep’s organs, looking around for a good spot to lay their eggs.
After the eggs are laid, a specific concentration of liquid disinfectant is used to clean them, allowing them to be sterilised yet yield a 70 to 80 per cent hatching rate.
Baptista said that checks are also performed on each individual batch of eggs to ensure that they are completely sterile before they are supplied to approved registered medical clinics and hospitals.
“This (manufacturing) process is approved and governed under the ISO13485 medical device directive, a global certification process for all medical devices.
“The Health Sciences Authority reviews the ISO audit results and approves the listing of our product on the national list of approved medical devices, as well as conducts random audits to ensure compliance to standards,” he added.
When the eggs hatch, live maggots will be ready to be dispatched in sterile vials, each containing around 200 tiny, writhing larvae.
“If a hospital calls us today and says it needs the maggots, we make the product ‘fresh’ by harvesting the eggs, cleaning and sterilising them, then placing them in transportation vials and incubating them overnight for supply in the morning the next day.
“When they arrive at the hospital, the maggots are fresh, hungry and ready to go,” he said.
Where the maggots have been used
At the department of rehabilitation at the National University Hospital (NUH), maggot debridement therapy has been used to treat four chronic wounds patients since August this year under a trial programme.
The treatment will be performed on suitable patient candidates from early next year.
NUH said that the cost ranges between $300 and $1,100 depending on factors such as the size of the wound, the patient’s response to healing and the amount of dressings required.
Older patients covered under the Pioneer Generation Package will be entitled to subsidies.
All four patients who underwent maggot debridement therapy at NUH this year were afflicted by lower limb wounds.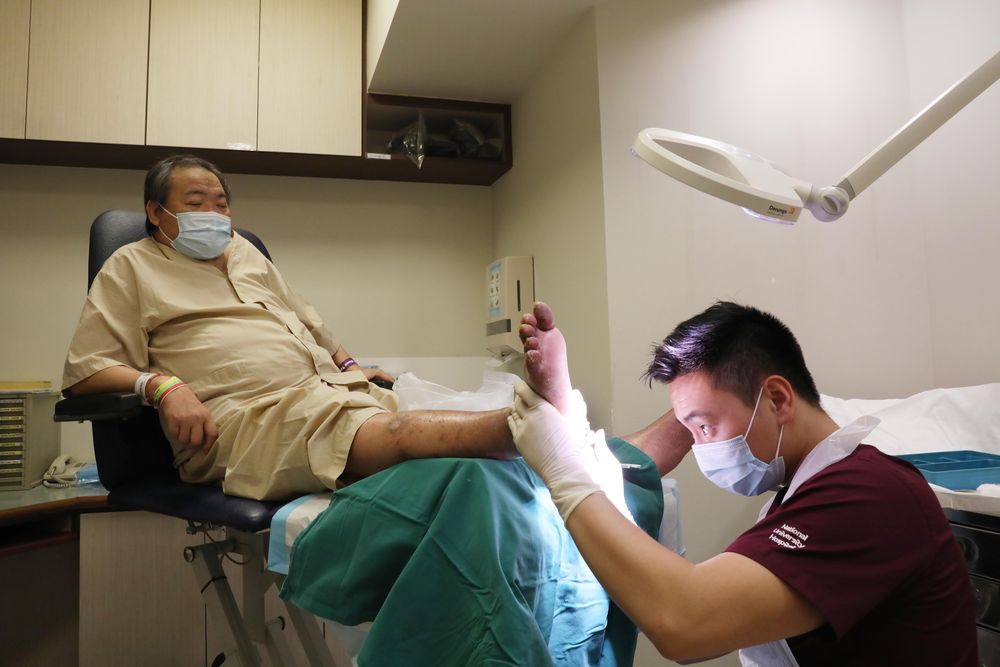
John Chen, a podiatrist at NUH’s department of rehabilitation, said that maggot debridement therapy is traditionally considered as a “last resort” treatment for salvaging limbs in patients.
However, this has changed after clinicians and wound care specialists began to understand more about its mechanism and therapeutic effects.
Patients with poor blood supply who may be deemed too high risk for surgery are considered good candidates for the therapy, Chen said.
Maggot debridement therapy is also available at Khoo Teck Puat Hospital (KTPH) but only for a selective group of patients.
Chelsea Law, a senior principal podiatrist and manager of the podiatry team at KTPH, said: “Patients who are suitable for the therapy are usually those with chronic wounds which are sloughy and may be too painful for podiatrists to perform bedside procedures.
“It is also useful for patients who are deemed too high risk for surgery but still need to ‘surgically’ remove devitalised tissues from their wounds.”
She added: “The value of maggot debridement therapy is that the treatment is selective and only devitalised tissues will be broken down by the enzymes excreted by the maggots, sparing the healthy tissue.”
The therapy has shown some clinical benefits in promoting wound healing and reducing the colonisation of some antibiotic-resistant strains of bacteria at the wound bed, but Chen of NUH emphasised that it is only one component of multidisciplinary wound care.
“Maggot debridement therapy should not be seen as a single treatment that will prevent (limb) amputation. Extensive medical and surgical care are critical in ensuring best patient outcomes,” he said.
In Teo’s case, he would likely have to undergo other procedures to improve his wound healing, Chen said.
How maggots help to promote healing
Maggots used in the therapy are placed directly in the open wound after it is cleaned with saline.
Technically speaking, the maggots do not “bite” when they are feeding.
On the wound, they seek out pockets of unhealthy or infected tissues and produce a fluid that liquefies them before sucking it all up, Baptista said.
Specialised dressings are used to keep the maggots in place during the treatment cycle, each typically lasting around 48 hours and not more than 72 hours.
Chen of NUH said that to achieve a clean wound bed, a patient might require two to five cycles, depending on the progress.
“Once we apply the maggots (on the wound), they do their job and we see them again in about two days’ time.
“After a cycle is completed, we remove the maggots and assess the wound response. At that point, if we think the wound is still not clean enough, we may consider doing more cycles.”
Will the free-roaming maggots escape from the wound during the treatment cycle?
“The maggots, it’s surprising, they don’t tend to escape from the wound because all their food is actually on the wound bed,” Chen said.
“So, they are attracted more to the wound than escape to other areas.”
Baptista said that after feeding on necrotic tissue, the maggots fatten up and usually increase 20 to 30 times their original size, depending on the amount of dead tissue consumed.
Unused maggots are discarded as biohazard waste.
Is there a risk of having the maggots turn into flies in patient’s wounds?
Baptista explained that this will not happen because the maggots are removed 48 to 72 hours, before they reach the next critical stage of its natural life cycle of becoming a pupa.
This is when they stop feeding and will look for a dry place to pupate.
Maggots for home care, in ‘bags’
Chen said that in general, the risks of maggot debridement therapy involved are “quite low”.
They may include bleeding, some pain and discomfort from the movements of the maggots on the wound bed.
During the treatment, patients can still move around, go to the toilet and wash up as long as they keep the wound dressing dry and clean, Chen said.
Maggot debridement therapy is usually done as an inpatient treatment. However, Baptista said that the treatment has also been carried out in home settings here.
Cuprina has facilitated more than five home-care maggot debridement therapy applications this year. They were prescribed by licensed clinicians in private practices, he said.
Besides the “free range” maggots that are applied directly onto a chronic wound, Cuprina also supplies maggots that are sealed in a fabric bag, much like a teabag.
Referring to them as “baggots”, Baptista said that the maggots cannot leave the confines of the bag and feed only through the perforations in the fabric.
‘The maggots cleaned up everything for me’
Among the NUH patients who underwent maggot debridement therapy this year is 58-year-old William Teo, who had a gangrenous wound in his right heel that was growing larger and worsening by the day.
Teo has diabetes and is undergoing dialysis for kidney problems.
He previously underwent surgery on his right heel at another hospital but the wound did not heal. It worsened and turned black after the operation.
Despite his initial apprehension of having live maggots placed into his wound, he decided to give the therapy a go at NUH after thinking through it for a day.
“At first, I was frightened. When they put the maggots in, I don’t know whether got pain or not,” he said.
“But it feels ‘normal’. I feel it when they eat (the flesh)… there’s a bit of pain like ants biting you. It’s not that painful.”
Teo underwent five cycles of the treatment, which took about a week-and-a-half.
He was pleased to see the “bad, brown tissue” progressively disappearing when he compared before- and after-treatment photos of his wound.
“They (the maggots) cleaned up everything for me,” he said. — TODAY






















