NEW YORK, Oct 18 — The morning after Christine Grounds gave birth to her son Nicholas, she awoke to find a neurologist examining her baby.
It was summer 2006, and Nicholas was her first child. There had been no indication that anything was wrong during her pregnancy, but it was soon clear that there was a problem.
“Did you know he has microcephaly?” she remembered the doctor asking matter-of-factly.
Confused, she replied, “What is microcephaly?”
This was before the Zika virus had spread from Brazil across South and Central America and the Caribbean and reached Florida. It was before doctors had determined that the virus could cause microcephaly, a birth defect in which children have malformed heads and severely stunted brain development. And it was before people had seen the devastating pictures of scores of newborns with the condition in Brazil and elsewhere.
Grounds, a 45-year-old psychotherapist, and her husband, Jon Mir, who live in Manhattan, had no idea what microcephaly would mean for them or for their child.
“We had a diagnosis but no prognosis,” recalled Mir, 44, who works in finance.
The doctors could offer few answers.
“We don’t know if he will walk,” the couple recalled being told. “We don’t know if he will talk. He might be in a vegetative state.”
But the truth was, even the doctors did not know.
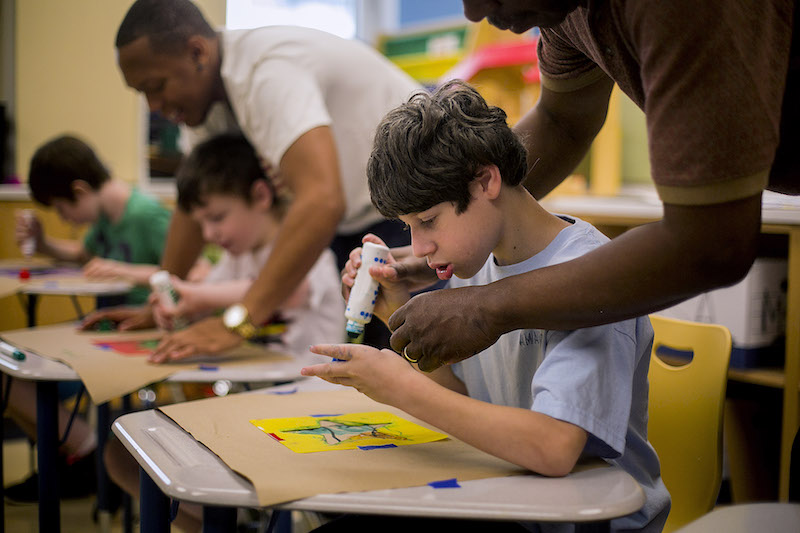
As mosquito season draws to a close in much of the country, taking with it the major risk of new Zika infections, there are still more than 2,600 pregnant women who have tested positive for the virus in the United States and its territories, according to the Centres for Disease Control and Prevention. They, and thousands more around the world, face the prospect of giving birth to a child with microcephaly.
Like other neurological disorders, microcephaly runs along a spectrum and its severity can vary widely. Zika-related microcephaly is believed to be somewhat different from microcephaly caused by genetics or other factors, but the result is largely the same: mental impairment that can run from mild to devastating. Detecting the condition before a child is born remains difficult and often impossible until very late in pregnancy — a fact that has renewed and fuelled political debates about abortion and made an already difficult choice for prospective mothers even more agonising.
Watching the unfolding epidemic and concerned that many people did not grasp what it meant to raise a child with microcephaly, Grounds offered to share her family’s experience.
“I was hysterically crying all the time,” she recalled of her son’s early days.
By the time Nicholas was 2, his developmental problems started to become evident. He crawled awkwardly, did not start to walk on time and would not make eye contact with others.
Fortunately, New York City has a robust early intervention programme for toddlers with developmental problems, and Nicholas was able to get special instruction and care.
Unfortunately, that care ends after three years.
While the city’s special education programme in the public school system gets generally high marks for helping children with conditions like autism, it is exceedingly difficult to provide the kind of care needed by children like Nicholas.
“A child with microcephaly needs scaffolding around every aspect of his life,” Mir said.

This summer, the CDC and the American Academy of Paediatrics published interim guidelines on how to evaluate and care for infants born with Zika-related microcephaly. They include a coordinated evaluation by multiple specialists within a baby’s first month of life, and then additional assessments of vision, hearing, feeding, growth, and neurodevelopmental and endocrine function during the first year. Families and caregivers also need support.
The CDC put the cost of care for each child at US$10 million (RM40 million) over a lifetime.
Grounds is quick to note that her family is more fortunate than many others because they can afford for Nicholas to get the best possible care and to enroll him at Manhattan Star Academy, a private school on the Upper West Side.
When Nicholas, who shares his father’s surname and is often called Nick, entered school, he was 5 and could barely communicate, mostly grunting and pointing.
“He couldn’t even close his mouth,” Kevin McManaway, a clinical coordinator at the school, said. A full day could be spent on reinforcement techniques to control his drool and keep his mouth closed.
In year three at the school, when Nicholas was 8, he started to combine words. For instance, he could say, “boy-eat.” But he could not communicate his own desires.
The breakthrough came in his fourth year. Just as he was getting started on a new communication device, “it was like a switch went off,” McManaway said.

Nicholas would exclaim: “Look the blue car. Throw ball. Jump. Get a haircut.”
McManaway said, “He just had this burst of language.”
Now, sitting in an art class, Nicholas is quick to say hello to a visitor and attentive to his teacher. On the playground, he grabbed a basketball and shot hoops, sinking as many as he missed. He is quick to offer the ball to others and to join in games. He is nothing like the child he was six years ago, his instructors say.
But all the progress came only after years of intensive and expensive intervention, and there is much work yet to be done to ensure that he has as full a life as possible.
On a weekly basis, Nicholas sees roughly a dozen different specialists and teachers, all concentrating on different parts of his development.
Every week at school, he has speech therapy four times, occupational therapy three times, physical therapy three times, individual counseling once, adaptive physical therapy twice, yoga once, and art class and music class twice each.
At home he receives more speech therapy, as well as additional physical and occupational therapy. Recently, he has also been able to participate in a variety of recreational activities.
Dr Wendy K. Chung, director of the clinical genetics programme at Columbia University Medical School, has spent years working with children with neurological development issues. She said people with microcephaly needed care beyond childhood.
“They need support their entire lives,” she said. — The New York Times






















