KUALA LUMPUR, July 11 — “It’s choosing who lives, then you know who will die. You come home and cry in the shower. Then you cry when you call the patients’ families. Then you cry when the patients die,” said a doctor at a government hospital here.
After more than a year of treating Covid-19 patients, doctors and nurses in Klang Valley hospitals are now forced to practice triage — assigning degrees of urgency to decide the order of treatment — on incoming patients.
Official reports of hospitals struggling to cope do not seem to truly reflect what is happening inside these hospitals.
The medical frontliners working here are prohibited from sharing any information with the media or public as civil servants are not allowed to do so under General Orders.
But in the past month, some have decided to speak up albeit anonymously.
“The situation is bad,” said another government doctor.
She said that manpower and hospital spaces are severely lacking, while cases continue to pile in daily, resulting in tortuously long waiting hours for those who are already sick.
A check at four government hospitals in Sungai Buloh, Ampang, Selayang and Kuala Lumpur showed that everything seemed to be under control.
At one of the hospital’s emergency departments, patients were being seen in a timely manner as they arrived.
Outside though, activity bordered on the hectic with ambulances rushing in and out ferrying patients.
On July 10, Malaysia recorded the highest Covid-19 cases in a single day with 9,353 cases, surpassing 9,180 cases recorded the day before.
Out of 9,353 cases, more than 50 per cent were found in Selangor with 4,277 cases and 1,398 cases in Kuala Lumpur.
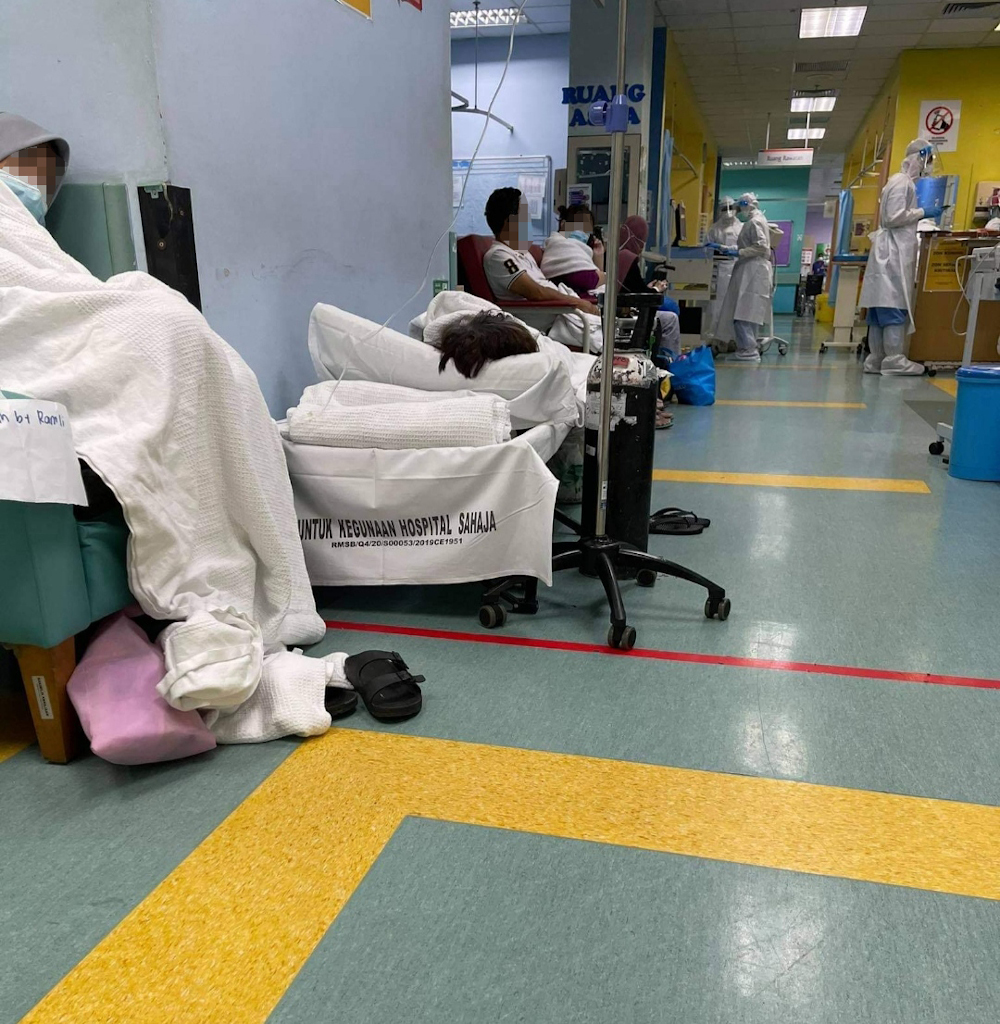
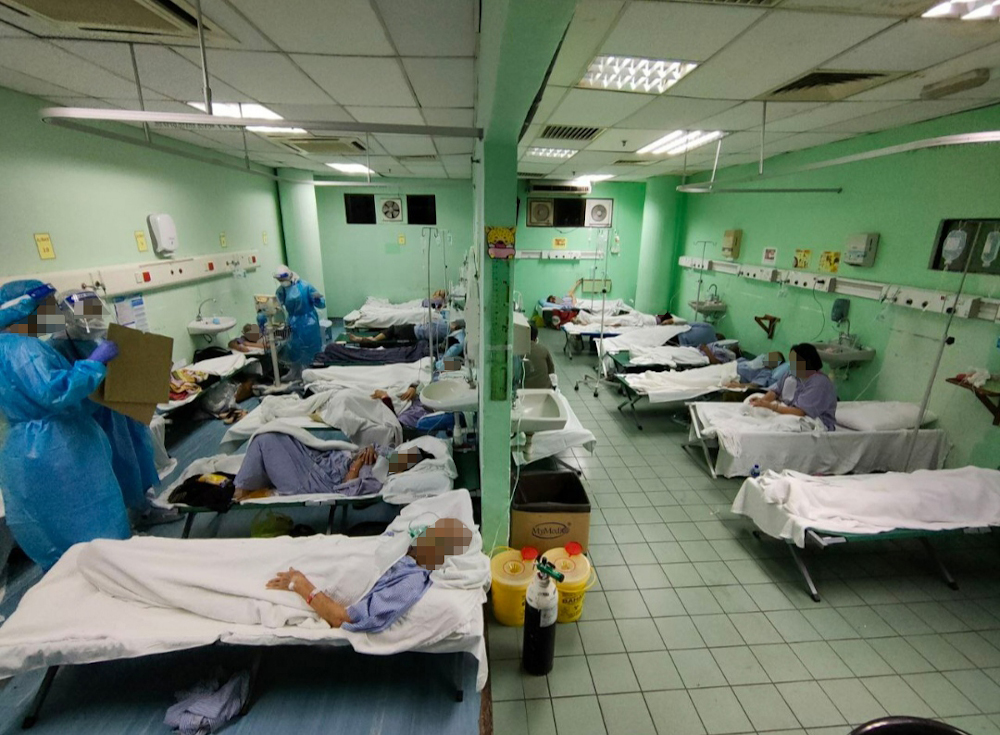
A medical officer at one of the hospitals said the situation has gone from bad to worse, with patients placed along its hallways on foldable camping beds.
”I can say that it’s the Klang Valley hospitals that are affected, but I can’t say all others are not affected,” she added.
Another doctor at another hospital told Malay Mail how she manages her Covid-19 patients when it came to oxygen distribution to save their lives, a task which involves her regularly consulting the hospital’s engineer.
”If I want to intubate a patient, or start a high flow nasal cannula on the patient in the ward, I have to calculate the total oxygen flow of the ward and check with the engineer what the ward’s capacity is.
“High flow nasal cannula is a non-invasive ventilator. But it uses super high flow oxygen, which explains the name, up to about maximum of 60 litres of oxygen,” she explained.
However, the 60 litres of oxygen is only enough to cater to one patient. If the maximum oxygen flow for the said ward is at 200 litres, that would only leave her with 140 litres for the others. Approximately 30 others.
So, how are a Covid-19 patient’s chances at survival determined?
“So now when the patients are referred to me, I will see what the comorbidities are like. Do they have any underlying issues such as diabetes, hypertension and others such as heart disease, kidney disease and whether they are obese, because all these are risk factors.
“Secondly, I will also look at their social support. Does this person have a family? Because most of the patients who are intubated probably would need a tracheostomy, so who is going to take care of the patient after that, you see?
”Or what is their premorbidity? Which means what was this person able to do, before this person got ill? If this person couldn’t even go out and walk or climb stairs, that means they are not that fit.
“Then I would definitely choose a younger patient to save compared to this patient. So, some patients who have got bad premorbidity, we actually tell their families that we would not be intubating their family members and probably this is the end.
“That’s why when they say it is like playing god... it is not easy, because you have to live with the fact that you chose someone’s life and you basically sentenced someone to death,” the doctor explained.
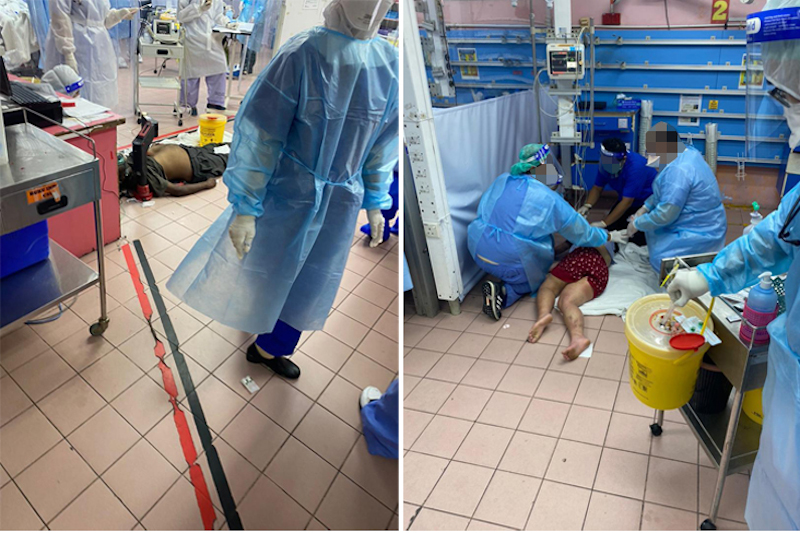
But the worst does not stop there, as patients who suffer from other critical, non-infectious diseases are also exposed to the risk of contracting Covid-19 at these hospitals.
“There is one thing we need to be reminded of when we deal with Covid patients: non-Covid-19 patients also suffer, as we have to redesignate resources,” explained another doctor.
Another medical frontliner told about a government hospital here that was recently in need of oxygen tanks, as the number of patients had ballooned beyond control.
“It was via a message that came to me and I verified, and I was told the oxygen situation is true.
“We are not blaming anyone, but if you use logic and rationale, people are making makeshift beds and based on the vacancies, there are only so many oxygen points available.
“So I work on my own deductions and messages from colleagues who are working at that hospital, that came to me. Even if there is no shortage now, we would definitely need it in the future,” the doctor said.
Meanwhile, many of these frontliners are getting infected as well despite being fully vaccinated.
A contract nurse with the Ministry of Health (MoH) shared her ordeal, after contracting the coronavirus from her patient.
The nurse who has since been discharged from a government-operated quarantine facility, said she felt dejected by the way she was treated.
“They said I am not really critical and do not need admission. I can accept that, but they cannot simply ask my family to fetch me and not assist me in finding a quarantine centre. This is nonsense and they have no empathy towards me.
“Don’t tell me that my uncle and brother who are not positive should take care of me? I scolded them... I told them I am a frontliner,” she said.
When frontliners are emotionally and physically drained, empathy is in short supply. A doctor who wrote in recently to Malay Mail said it best:
“Patient care also suffers in other ways when a doctor is exhausted, emotionally detached: there is a lack of connection, a sense of being cared for, of being heard.”



















