KUALA LUMPUR, Feb 27 — Malaysia’s handling of the Covid-19 outbreak has earned the country much praise, both locally and internationally.
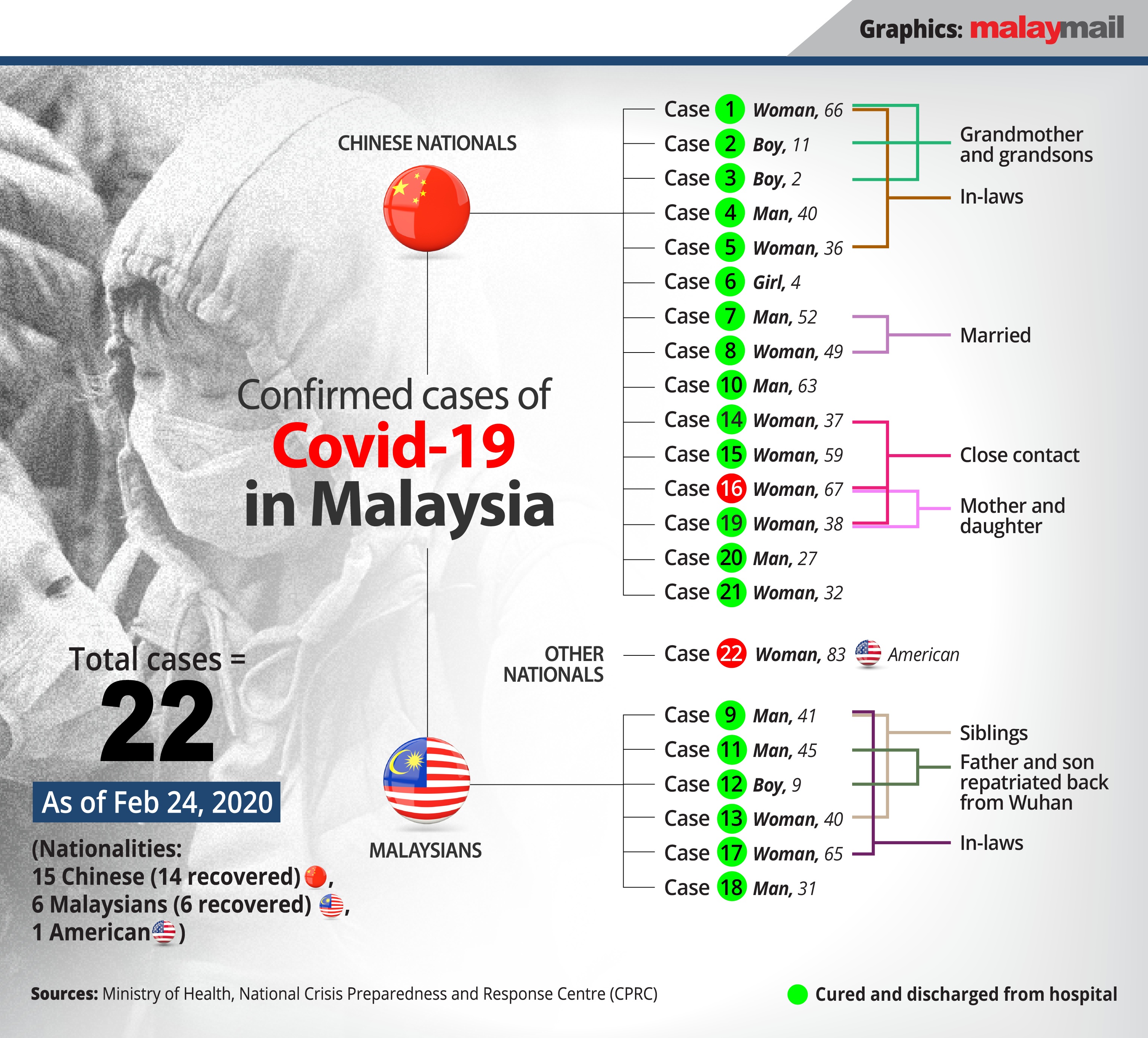
Total cases to date remain at 22, with zero fatalities, 20 fully recovered patients, two stable in hospital, and no new cases since February 15, health authorities announced yesterday evening.
The effort to keep the numbers from growing speaks volumes of the level of dedication and coordination among the country’s various medical and disaster management agencies.
One such agency is the Institute of Medical Research (IMR). Its responsibility is widespread and covers running diagnostics, research, consultancy, and training pivotal in combating the spread of diseases — be it viral, bacterial or parasitical.
Malaysia’s battle to contain the novel coronavirus from becoming an epidemic like the city of Wuhan in China began as early as January 3, according to virology unit head Dr T. Ravindran, who is also part of IMR’s Infectious Diseases Research Centre (IRDC), yesterday.
“We began preparing as early as January 3, and by January 21 the reagent to identify Covid-19 arrived at IMR’s labs.
“The following day real-time optimisation tests were successfully conducted and the reagent provided to the national public health lab in Sungai Buloh which was important in identifying the first contact-case,” he told reporters during a media tour of IMR’s facilities on Jalan Pahang here.
Dr Ravindran said IMR laboratories could determine the presence of Covid-19 from samples within as few as five to six hours.
Alongside IMR director Dr Tahir Aris and IRDC chief Dr Norazah Ahmad during the tour, Dr Ravindran explained the step-by-step processes to identify the presence of Covid-19 in clinical samples.
“Firstly the samples arrive from the hospitals and are recorded in the database, and aliquots are taken for the purpose of deactivating the virus. This is followed by deactivating the samples themselves, and extracting its ribonucleic acid.
“After this comes the preparation of the real-time reverse transcription polymerase chain reaction (RT-PCR) reagents, and the real-time RT-PCR tests on Covid-19. The results are analysed, and must usually be reported immediately to the Health Ministry’s Crisis Preparedness and Response Centre,” he said.
IMR has two physical locations. The second is in Setia Alam, Selangor.
Dr Ravindran said out of a total 700 or more IMR personnel, 18 from his unit are in the the Setia Alam facility which focuses on research, while the Jalan Pahang facility has 38 members of his unit who mainly conduct diagnoses.
 “In the event of an outbreak, we can have people coming in from Setia Alam. For particularly severe instances, all 56 IMR virology unit personnel will be roped in. We also conduct outbreak investigation as and when it is needed.
“In the event of an outbreak, we can have people coming in from Setia Alam. For particularly severe instances, all 56 IMR virology unit personnel will be roped in. We also conduct outbreak investigation as and when it is needed.
“The ministry usually requires our assistance for the public health labs who conduct surveillance activities. In addition, we work alongside the National Disaster Management Agency and other bodies, where meetings are held regularly so that everyone is on the same page and prepared should an outbreak occur,” he said.
On an ordinary day, Dr Ravindran said IMR virology unit personnel conduct routine diagnostics for things like influenza, HIV or the varying types of hepatitis. At present, unit staff who are not on call to handle Covid-19 continue to perform routine diagnosis and lab analyses.
In his 27-year career with the institute, the virologist said he has witnessed many instances of outbreaks, with one example being the Nipah virus in 1998 and 1999, which resulted in 105 deaths and the culling of over a million pigs by the authorities to stem the spread.
“It was not so widespread since it happened in pig-farming areas, and was confined to certain individuals only (such as pig farmers). But the real challenge for us was the 2009 influenza pandemic, when a lot of samples began to come in rapidly. At the time IMR was the only lab providing its services for the whole country.
“At its peak, we were receiving up to 600 samples daily. Though we managed to overcome this challenge, the pandemic was a turning point as we realised things could not continue the way they were,” he told Malay Mail later, after the tour ended.
Since then, Dr Ravindran said testing for viruses has been decentralised, with 12 hospitals and five national public health labs nationwide able to conduct similar testing, which has made the response and handling of Covid-19 much easier.
“We are also boosted by the support from private labs, as some may prefer to go to the private sector for any sort of infection. When Covid-19 arrived on our shores, we acted quickly and provided training for hospital personnel, which took some of the burden off our shoulders since they can do the testing instead of us alone.
“Looking back at things, IMR has ended up in a far better position than it was over a decade ago. We did not sit by idly but instead learned from our experiences and put them into action. As far as we are concerned, the ministry is very well prepared for any eventualities that may arise,” he said.
Despite the institute’s tireless efforts in combating the spread of Covid-19, Dr Ravindran chooses to remain modest, adding that IMR is not alone in this.
“Everyone has got their own roles to play, the importance of others including the public health labs cannot be understated. With all of us fulfilling our niche roles, handling outbreaks and pandemics becomes all the more efficient,” he said.



















